Pre-Eclampsia: What We’re Not Told — And What Actually Helps
Women’s Health is playing a big catch up right now.
Until recently we were left out of trials, crash test dummies were based on male bodies and pregnancy advice has been based on Male ideology, not science.
This was not because women are rare or complicated,
but because the research simply wasn’t been done.
The gaps are not biological — they’re political, cultural, and historical.
Women’s bodies have been systematically underfunded,
under-studied, and under-valued in medical science for generations.
Pregnancy research, especially, is decades behind where it should be.
Even when new findings do emerge, they don’t reach women quickly.
In healthcare there’s a well-documented delay of around 17 years between research evidence and actual implementation in guidelines or everyday practice.
Seventeen years.
That means the things we now understand about:
placental development
stress physiology
metabolic health
continuity of care
blood volume expansion
nutrition and micronutrients
the role of inflammation and oxidative stress
…simply aren’t reaching women in time.
They sit in journals while maternity services remain overstretched,
cautious, and often trapped in outdated models.
So we end up with this strange mismatch:
there is a huge amount of research now, but it rarely makes it into clinical conversations.
As a result, women are still often led to believe that pre-eclampsia is random, mysterious, or purely genetic.
The official NHS leaflet lists a handful of medical risk factors — but says almost nothing about physiology, nourishment, stress, or the lifestyle factors that help women support their own outcomes.
Massive areas of pregnancy physiology that affect half the population remain poorly explained, quietly ignored, or reduced to a simple risk list.
Mainstream maternity care is excellent at monitoring problems,
but it rarely offers the tools that actually strengthen health or reduce the strain on a woman’s system.
This is the context in which we have to talk about pre-eclampsia.
Not as an isolated medical condition, but as something deeply linked to how women are cared for, nourished, supported and listened to.
It’s serious, it’s common, it’s widely monitored
— yet most women are given only the shallowest explanation of what it actually is.
Modern research has moved far beyond this simplistic narrative.
Pre-eclampsia isn’t random, and while nothing in biology is ever fully preventable,
there are ways to reduce strain on the body and support the systems involved.
This blog brings together what the science says,
what traditional birth work has observed for generations,
and how nourishment, rest, nature, community,
and continuity all help create a healthier pregnancy environment.
I’ll link to my other articles where relevant so you can explore the practical details more deeply.
I don’t promise cures
- I am here to blend the scientific evidence and traditional wisdom,
to help you take charge of your own health and pregnancy journey.
How Common Is Pre-Eclampsia
— And Is It Random?
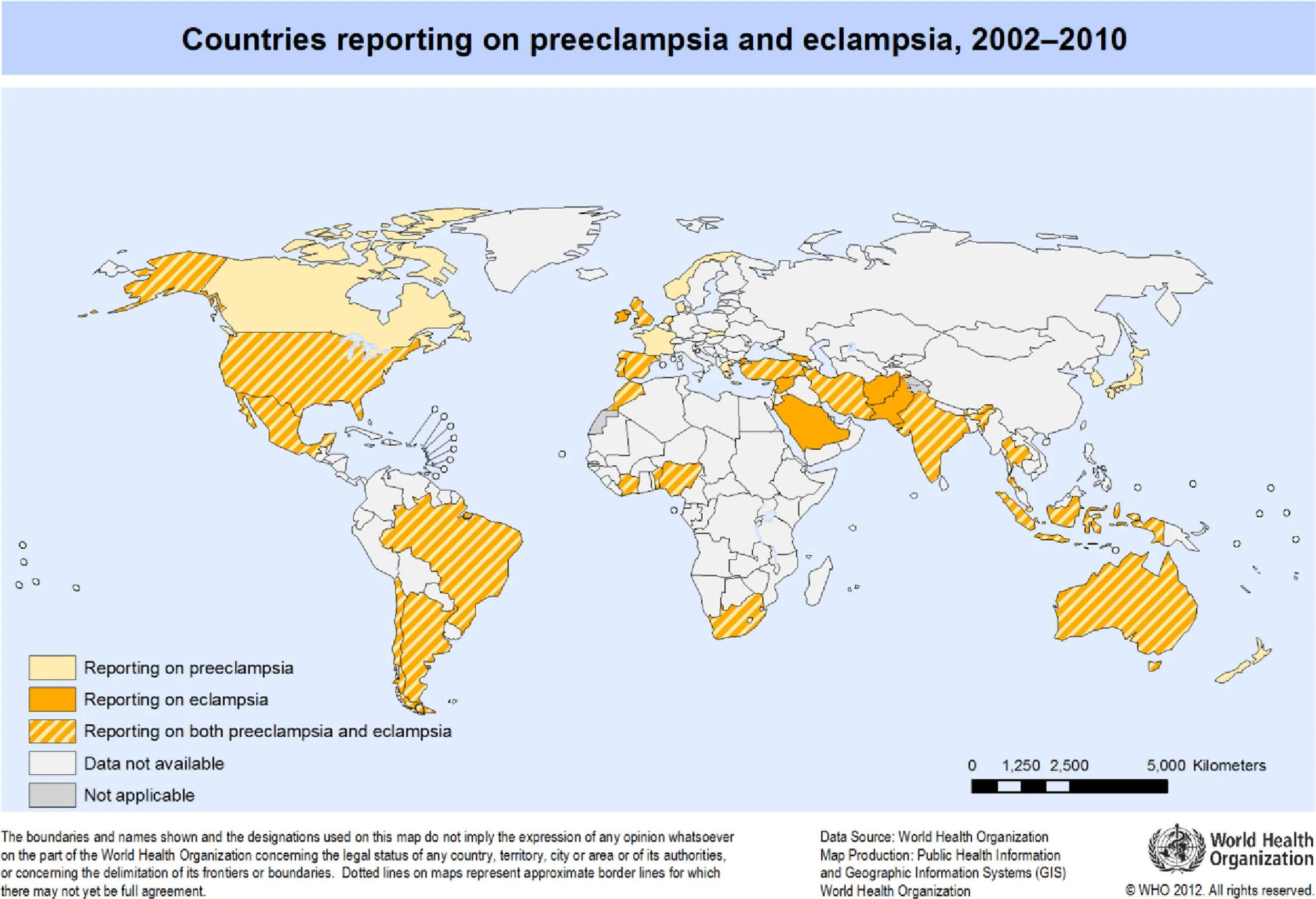
Worldwide, pre-eclampsia affects around 2–8% of pregnancies, and 3–5% in the UK (NICE NG133; MBRRACE)⁽¹⁻²⁾.
But crucially, it is not distributed evenly.
It occurs more frequently in:
women experiencing chronic stress or adversity⁽³⁾
women facing nutritional depletion or low metabolic resilience⁽⁴⁾
first-time mothers⁽³⁾
women who have had it before⁽³⁾
women with cardiovascular or metabolic strain⁽⁴⁾
Black women — due to systemic pressures, racism and cumulative stress exposure, not genetics⁽⁵⁾
If pre-eclampsia were genuinely random,
none of these patterns would exist.
Antenatal care is excellent at detecting pre-eclampsia
— but it does not add health or continuity.
This is where women often fall through the cracks:
because monitoring alone cannot lower stress hormones,
nourish blood volume, or support the nervous system.
Continuity of care has been shown to reduce hypertensive disorders,
including pre-eclampsia (Cochrane Review, Sandall et al.)⁽⁶⁾.
Not because symptoms are spotted earlier,
but because physiology changes when women feel supported and known.
When NHS continuity isn’t available,
Independent Midwives and birth-keepers provide
the steady companionship that research keeps showing protective effects for.
So What Is Pre-Eclampsia?
Pre-eclampsia starts in the placenta, not in late pregnancy.
The first trimester is where the early mechanism begins.
Normally, the placenta remodels the uterine arteries so blood can flow freely.
In pre-eclampsia, this remodelling is incomplete, limiting blood flow and creating a hypoxic, stressful environment (Redman & Sargent; Roberts & Hubel)⁽⁷⁻⁸⁾.
A stressed placenta releases inflammatory and anti-angiogenic signals into the mother’s bloodstream.
These signals make her vessels:
tighter
more reactive
more inflamed
more “leaky”⁽⁷⁾
Over time, this appears as:
high blood pressure
protein in the urine
swelling
headaches, visual changes
abnormal liver and kidney markers
clotting disturbances⁽⁷⁻⁹⁾
This is why it’s not random: the mother’s overall environment (stress hormones, inflammation, metabolic health, nutrient status, sleep, social pressure) amplifies how strongly she responds to placental signals.
What Happens If Pre-Eclampsia Isn’t Treated?
If the condition progresses unchecked, it can escalate into:
severe hypertension
HELLP syndrome
eclampsia (seizures)
placental abruption
organ injury
fetal growth restriction
reduced amniotic fluid
preterm birth
stillbirth in severe cases⁽¹⁰⁻¹¹⁾
Monitoring is essential
— but again, it does not build health.
It only flags when the system is struggling.
What Actually Helps: The Real Foundations for a Healthier Pregnancy
Nothing guarantees prevention.
But many things genuinely support vascular health, immune balance, blood volume, metabolic stability, and the nervous system — all of which influence how pregnancy unfolds.
These are the most effective, accessible foundations.
1. Pregnancy Yoga & Yoga Nidra
Yoga reduces inflammation, improves circulation and regulates blood pressure (Field et al.; Beddoe et al.)⁽¹²⁻¹³⁾.
Yoga Nidra in particular lowers cortisol and supports parasympathetic rest (Moszeik et al.)⁽¹⁴⁾.
Reduced stress and improved autonomic balance directly influence endothelial function and placental blood flow (Sorensen et al.)⁽¹⁵⁾.
Community connection during classes also improves oxytocin levels and reduces maternal stress
— both protective in pregnancy.
2. Hydration With Spring Water
Blood volume must increase by ~50% in pregnancy (Brown & Lindheimer)⁽¹⁶⁾.
Hydration is a key driver of this expansion.
Spring water supports:
natural electrolytes
mineral balance
chemical-free hydration
And the act of collecting water
— moving, grounding in nature —
reduces stress hormones (Wadhwa et al.)⁽¹⁷⁾.
For local, ancient & traditional, trusted water sources in The Forest of Dean click below:
3. Real Nourishment:
Protein, Minerals, Salt, Calories & Animal Foods**
(Brewer-inspired + backed by physiology)
Healthy plasma expansion requires:
adequate protein
salt
minerals
calories
whole foods⁽¹⁶⁾
Protein needs during pregnancy range from 80–100g/day, more for twins (Kaiser et al.)⁽¹⁸⁾.
Salt restriction is outdated and can worsen pregnancy outcomes
(Leduc et al.)⁽¹⁹⁾.
Animal foods provide:
choline
B12
haem iron
DHA
retinol
essential amino acids
minerals
(These nutrients are under-consumed and critical for blood volume and placental development)⁽¹⁸⁾.
Many women instinctively crave eggs, butter, broth, fish or meat — the body signalling its needs.
More detail is in my nutrition article here:
4. Leafy Greens for Oxidative Stress
Oxidative stress plays a key role in the development of pre-eclampsia
(Burton & Jauniaux)⁽²⁰⁾.
Leafy greens provide antioxidants and micronutrients that support endothelial health
(Roberts & Bodnar; Rumbold et al.)⁽²¹⁻²²⁾.
Daily intake of:
kale
parsley
spinach
chard
herbs
sea greens
provides gentle, consistent antioxidant support.
5. Continuity & 1:1 Support
The Cochrane Review on midwife-led continuity
shows lower rates of hypertensive disorders,
including pre-eclampsia
(Sandall et al.)⁽⁶⁾.
Other major studies confirm:
reduced complications
improved physiological outcomes
lower intervention rates
higher maternal satisfaction⁽²³⁻²⁴⁾
The mechanism isn’t “better surveillance.”
It’s lower stress.
Chronic stress tightens blood vessels, increases inflammation, and disrupts placental signalling (Coussons-Read; Jauniaux; Wadhwa)⁽²⁵⁻²⁷⁾.
A birth-keeper or Independent Midwife offers:
consistent emotional support
relational safety
deep listening
practical guidance
evidence-based advice blended with traditional wisdom
Continuity regulates the nervous system — and that directly protects physiology.
If you’re considering 1:1 continuity,
I’m happy to support you or help you find someone aligned if I’m unavailable.
Bringing It All Together
Pre-eclampsia begins early in placental development and emerges more strongly in bodies and environments under strain.
Nothing prevents it with certainty, but many things support the systems involved: nourishment, rest, stress reduction, continuity, hydration, antioxidant-rich foods, and nervous-system stability.
Medical care monitors problems — but it does not build health.
That’s where community, relationship-based support, and traditional pregnancy wisdom become essential.
If you want to explore deeper support — or need help finding a birth-keeper or IM — you’re welcome to get in touch.
Women deserve information, continuity and nourishment, not just monitoring.
References & Further Reading
Pre-eclampsia incidence & risk factors
National Institute for Health and Care Excellence (NICE). Hypertension in Pregnancy: Diagnosis and Management. NG133 (2019).
Tranquilli et al. The Classification, Diagnosis and Management of the Hypertensive Disorders of Pregnancy: ISSHP Statement. Pregnancy Hypertension (2014).
Knight et al. MBRRACE-UK Perinatal Mortality Surveillance Report. (Annual reports).
McDonald et al. Preeclampsia and Gestational Hypertension: Epidemiology and Risk Factors. Clinical Obstetrics and Gynecology (2022).
Tikkanen et al. Maternal Ethnicity and Hypertensive Disorders of Pregnancy. American Journal of Obstetrics & Gynecology (2023).
(Shows disproportionately higher rates in Black women, linked to systemic factors, not genetics.)
Pathophysiology of pre-eclampsia: placenta, oxidative stress, endothelial dysfunction
Redman & Sargent. Placental Stress and Pre-eclampsia: A Revised View. Placenta (2009).
Roberts & Hubel. The Two-Stage Model of Preeclampsia: Variations on the Theme. Placenta (2019).
Burton et al. Hypoxia, Oxidative Stress and Placental Development. Journal of the Society for Reproductive Investigation (2021).
Staff et al. The Vascular Biology of Pre-eclampsia. Hypertension (2013).
Effects of untreated pre-eclampsia
Sibai et al. Maternal and Perinatal Outcomes Associated with Severe Preeclampsia. Obstetrics and Gynecology (2005).
Chappell et al. Pre-eclampsia: Contemporary Management. BMJ (2021).
Nutrition, blood volume expansion, protein, Brewer-aligned principles
(Note: Brewer’s original work is historical and controversial; the citations below support the physiological principles used, not his entire doctrine.)
Brown & Lindheimer. Volume Homeostasis in Normal Pregnancy and Pre-eclampsia. American Journal of Kidney Diseases (1999).
(Shows the importance of plasma expansion.)Leduc et al. Salt Intake and Pregnancy: Time to Reconsider? Hypertension in Pregnancy (2008).
(Evidence that salt restriction is harmful.)Kaiser et al. Protein Needs During Pregnancy. American Journal of Clinical Nutrition (2014).
(Supports increased protein requirements.)Harding et al. Nutrition and Placental Development. Reproduction, Fertility & Development (2015).
Leafy greens, antioxidants & oxidative stress
Roberts & Bodnar. Antioxidants and Pre-eclampsia. American Journal of Obstetrics & Gynecology (2007).
Burton & Jauniaux. Oxidative Stress in Pregnancy. BJOG (2011).
Rumbold et al. Green Leafy Vegetable Intake and Pregnancy Outcomes. Nutrition Reviews (2013).
Omega-3 fatty acids & reduced hypertensive disorders
Olsen et al. Marine n-3 Fatty Acids and Risk of Pre-eclampsia. The Lancet (1992).
Mahomoodally et al. Omega-3 Supplementation in Pregnancy and Maternal Cardiovascular Health. Nutrients (2020).
Yoga, Yoga Nidra, stress physiology & blood pressure
Field et al. Yoga and Pregnant Women’s Health: A Systematic Review. Journal of Perinatal Education (2012).
Beddoe et al. Yoga for Stress Reduction and Mood in Pregnant Women. Psychology & Health (2009).
Moszeik et al. Yoga Nidra: Physiological and Psychological Benefits. International Journal of Yoga Therapy (2021).
Sorensen et al. Stress Reduction and Blood Pressure in Pregnancy. Psychosomatic Medicine (2019).
Continuity of care reducing pre-eclampsia & hypertensive disorders
Sandall et al. Midwife-Led Continuity Models vs Standard Care. Cochrane Review (2016).
(Shows reduced hypertensive disorders, better outcomes, higher satisfaction.)Tracy et al. Continuity of Midwifery Care and Reduced Pregnancy Complications. The Lancet (2013).
Homer et al. Relationship-Based Care: Positive Impacts on Perinatal Outcomes. Women and Birth (2019).
Stress, cortisol, vascular reactivity
Wadhwa et al. Prenatal Stress and Placental Function. Current Directions in Psychological Science (2011).
Coussons-Read et al. Stress and Inflammation in Pregnancy. Journal of Reproductive Immunology (2013).
Jauniaux et al. Stress Hormones and Vascular Function in Pregnancy. Placenta (2017).